
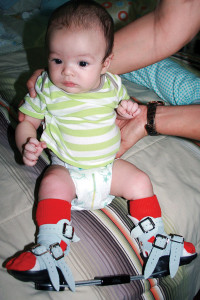
Photo courtesy of SureStep.
As hip arthritis becomes a growing concern in adults with Down syndrome, clinicians are also becoming more attuned to hip issues in children with DS in hopes that early intervention in the pediatric population will help reduce the risk of disability later on.
By Shalmali Pal
Based on the numbers alone, hip disorders in children with Down syndrome (DS) don’t seem to be a cause for great concern—it’s estimated that only 5% to 8% of this patient population will suffer from hip impairments, with the most common being subluxation.1 But the detrimental effects of hip disorders can have serious implications, most notably the development of early arthritis.
“Fortunately, [hip disorders] in children with Down’s are relatively uncommon. But when it’s bad, it’s bad, so you don’t want to outright dismiss it [as a possibility],” said Stephen England, MD, a pediatric orthopedic surgeon at Park Nicolette Health Partners in St. Louis, MN.
Orthopedic problems are the second most common cause of disability (after cardiac issues) in adult patients with DS, who are living more active, longer lives (See “Down syndrome and total hip arthroplasty: Opportunities to optimize outcomes,” LER March 2015, page 16).
“Now that cardiac issues, such as coronary artery disease, are being identified and treated more aggressively, and because the lifespan of children with DS is longer, these [orthopedic] problems will definitely be more of an issue for the adult DS population,” said Stephen Sundberg, MD, a pediatric orthopedic surgeon and program medical director of the Center for Pediatric Orthopedics at Gillette Children’s Specialty Healthcare in St. Paul, MN.
LER spoke with Sundberg, England, and other biomechanics experts about the diagnosis and management of hip disorders in children with DS.
Common causes
There are three main reasons for hip disorders in kids with DS. One of the least prevalent is Legg-Calve-Perthes (LCP) disease, where the head of the femur loses blood supply and the bone becomes weak and misshapen. This condition generally manifests in children aged 4 to 8 years as a painless limp and the loss of full range of motion in the hip.1 LCP occurs in children with and without DS, but data on how commonly it’s seen in the latter population are scant, according to England.
Then there is slipped capital femoral epiphysis—also known as epiphysiolysis, but generally called SCFE (pronounced “skiffee”)—in which the rounded head of the femur slides on the femoral neck. This hip impairment is linked with obesity and hypothyroidism. SCFE presents as a limp with associated pain in the hip or even the knee.1
“SCFE generally hits right around puberty,” explained Kathy Martin, PT, DHS, a professor and director of the Doctor of Physical Therapy Program at the Krannert School of Physical Therapy, University of Indianapolis. “Because this disorder is closely tied with the onset of puberty, we feel like there is some hormonal element involved. So the increased load from being overweight plus hormonal changes may put some kids with DS at a greater risk for SCFE.”
Finally, there is subluxation, where the head of the femur moves out of the acetabulum.
“This dislocation may or may not be associated with malformation of the acetabulum. The dislocation appears to be due to a combination of laxity of the connective tissue that normally keeps the hip together along with the low muscle tone found in DS,” wrote pediatrician Len Leshin, MD, in a 2003 online article.1
Sundberg described subluxation as a deficiency in the posterior wall of the hip socket in children with DS.
“We think that the back wall of the socket is relatively underdeveloped, and that can predispose a small percentage of these kids to develop a progressive hip dislocation,” he said.
England added that subluxation can be painless, with the hip joint popping in and out of place.
“You or I would no doubt feel that, but for a child with DS, that ability to pop the hip out may become something they are accustomed to,” England said.
Sundberg emphasized that practitioners will need input from caregivers and parents to make the correct diagnosis.
“We generally find that kids with DS may not tell us if something is painful,” he said. “We have to rely on the families to give us the feedback. They’ll tell us that, ‘My child is behaving different. He used to be able to join us for family walks or was willing to come with me to the grocery store. Now he wants to stay at home and spends more time sitting.’”
Martin also stressed obtaining feedback from parents or other caregivers who know the child best. Just as parents can tell whether an infant’s cry means “I’m hungry” or “I’m tired,” they can offer insight into why a child is refusing a routine activity.
“They can often discern some of the subtle behaviors that may indicate a physical problem or may just mean, ‘I don’t want to do this today,’” she said.
Subluxation can manifest at any age. Ideally, pediatricians are assessing for potential hip dysplasia during wellness check-ups in all newborns and infants, the experts agreed. Accepted physical tests for dysplasia include the Barlow and Ortolani tests.2
Martin said subluxation is something she sees more often in infants and toddlers than in older children.
“Many orthopedic surgeons consider a congenitally dislocated hip as an orthopedic emergency. It needs to be addressed and treated immediately,” she said, or patients face poor outcomes, such as the early onset of hip osteoarthritis.3
If a hip disorder is suspected, the child can be sent for an orthopedic exam that may include x-rays. But England cautioned that a static x-ray may show a completely normal hip, as subluxation is a dynamic condition.
Arthrograms will reveal subluxation more readily, allowing clinicians to look specifically at the dynamic relationship between the femoral head and the cup, England said, “but arthrograms are not something you want to do routinely because they require anesthesia.”
He emphasized that before children with DS undergo any invasive procedure requiring anesthesia, they need to be checked for laxity in the cervical joints (C1/C2) as instability in those locations could lead to “potentially catastrophic” problems if the neck is hyperextended to accommodate intubation. These problems can include deterioration of gait, loss of manipulative skills, and hemiparesis.4
Sundberg added that assessing hip health in children with DS may require more vigilant observation than in a typical child. Hip subluxation goes through stages; a child may begin life with normal hips but can develop progressive subluxation over the course of many years, he said.
“The hip may be moving in and out of the socket, and the child may not complain of pain early on,” he said. “But they may ultimately go on to develop a fixed dislocation where the hip no longer wants to go back into the socket. That’s not a situation we want to leave unaddressed.”
The surgical approach
Are all children with DS and hip disorders candidates for surgery? There are numerous factors that go into making that call.
A 2006 review article5 on the role of the orthopedic surgeon in DS offered clear cut-advice: “In the absence of radiographic changes in a child whose hip dislocates, we recommend immobilization in a hip spica cast or hip abduction orthosis. When radiographic changes are evident in the acetabulum or when signs of subluxation of the hip are present, we recommend surgical intervention.”
However, Sundberg said he is not convinced that casting or bracing will keep patients out of the surgical suite. He explained that even with some level of success with nonsurgical methods to reduce subluxation, children with DS will still have progressive migration or shallowness of the hip socket.
“They are more than likely to end up needing surgery,” he said.
A Bernese periacetabular osteotomy (PAO) is the preferred surgical intervention to reorient the socket, Sundberg said. Studies have shown good success rates with PAO, with patients maintaining high Harris Hip scores at six months and one year postsurgery, as well as clinical stability and asymptomatic improvement at five years.6,7
Sundberg said his group has done the procedure in children with DS who were as young as 8 years.
“There’s an age range that depends upon when the instability develops,” he said. “If the kids are younger and have no open growth plates, then we may do the PAO. If subluxation becomes a problem as the kids approach skeletal maturity, ages twelve to fourteen, we may consider a standard, adult-style osteotomy.”
Caregivers need to be aware that surgical adjustment of subluxation in childhood is no guarantee that the patients won’t experience hip disorders in adulthood, England pointed out.
“The goal with the surgery is to prevent that joint from popping in and out, but the joint is still likely to wear out, which can lead to arthritis,”3 he said. “I don’t necessarily think [surgery] leads to long-term joint preservation; I think it’s more about short-term joint stability.”
Lengthen and strengthen
As with surgery, conservative treatment options for kids with DS and hip disorders depend on the type of impairment and the child’s age.
For infants with subluxation, the standard in conservative therapy is the Pavlik harness, which limits range of motion of the hip joint. Unlike a rigid cast, the harness allows the child to move freely within a certain range.
“It allows kids to flex and externally rotate, but it limits their ability to go into adduction,” Martin said. “It keeps them out of the end range of the position where the hip is likely to pop out.”
But the Pavlik harness is most successful in children aged up to 6 months. In a Turkish study of harness use for developmental hip dysplasia (DHH) in children with a mean age of 8 weeks, 18 of 31 procedures were deemed successful with no avascular necrosis at follow-up.8 A UK study of 123 hips treated in an infant DHH screening program found that all hips diagnosed with dysplasia or subluxation, but not dislocation, were managed successfully in the harness.9
If the subluxation isn’t discovered until the child is older, then a closed reduction under general anesthesia is likely necessary. The child is then put in a spica cast to keep the hip in position during healing.2,5
When it comes to getting the most out of noninvasive treatments, Martin said, “the earlier, the better,” as the development of the acetabulum is limited after the first 18 months of life.
“If the joint is still developing and remodeling, you can guide how it remodels and make it more stable in that first eighteen months,” she said. “If you’ve missed that window of opportunity, then you are limited as to what changes you can make in that joint.”
Those with LCP and SCFE are more likely to be candidates for surgery. In the case of LCP, the procedure will establish proper alignment of the hip bones. In the case of SCFE, surgery is a must as it will speed up the epiphysis closure.10,11
Of course, physical therapy (PT) is paramount for all patients, experts say, regardless of whether they’ve undergone correction with surgery, bracing, or casting.
The goal with PT in this group is not so much to impact the joints directly, but to “lengthen and strengthen” the muscles around the hip, balancing the muscles so that the hip remains centered in the socket. Martin pointed out that children with DS have what she called “a double whammy.”
“They have low muscle tone, and they have ligamentous laxity. The ligaments are the primary joint stabilizers, so if those aren’t working, then you rely on secondary joint stabilizers to protect the joints, and those are the muscles,” she said. “We are trying to make sure that there is optimal range of motion, and then maximizing the strength of the muscles to help support the hip.”
Feet first
The hypotonia or hypermobility that predisposes children with DS to hip disorders also is often manifested in the foot.12,13 Making the connection between better foot health and better hip health in the DS population has been a shortcoming in the medical community, according to Louis DeCaro, DPM, of the DeCaro Total Foot Care Center in West Hatfield, MA, who is also president of the American College of Foot and Ankle Pediatrics.
“I think that there are certainly many specialists that don’t consider the significant impact of the foot on short- or long-term hip health. I think that they see a lot of [kids with DS] where they make judgment calls about the hips, but don’t realize that the foundation has not been addressed well,” he said.
Martin agreed that addressing foot impairments in children with DS may often go unexamined, especially by general medicine practitioners.
“I think [addressing the feet] is becoming more common, with the idea of providing support as soon as kids with DS are showing interest in getting on their feet, but it’s PTs and developmental pediatricians who are initiating that,” she said.
Research showing causation between foot laxity and hip instability is lacking, but connections between ligamentous laxity and musculoskeletal disorders have been demonstrated. A 2004 study looked at 125 children who presented at a pediatric rheumatology clinic with painful conditions related to hypermobility. The authors reported that the majority of the patients had pes planus and muscle weakness. Of the total population, 12% had what the authors called “clicky” hips at birth, and 4% had a congenital dislocatable hip.13 A 2013 article from Gillette pointed out that “excessive ankle joint laxity and pes planus are more common in patients who have joint hypermobility.”14
“I think about alignment of the whole lower extremity,” Martin said. “If you help align the foot, then everything stacks up better. [For] a child with a collapsed arch or pronated foot—it’s like driving a car with the front end out of alignment. The car will move, but there’s going to be abnormal wear and tear.”
Treatment options for foot problems in children with DS include flexible supramalleolar orthoses (SMO) or custom foot ankle orthoses.
In children with DS and hypotonia (mean age approximately 6 years), Martin reported significant improvement with SMOs versus shoes only for the standing, walking, running, and jumping dimensions of the Gross Motor Function Measure. Results were seen immediately and after seven weeks of use.15
In another study in children with DS aged 3 to 6 years, wearing custom foot orthoses was associated with decreased ankle eversion during static standing, and various improvements during walking, such as a decreased foot progression angle and a change in the initial contact site from flat foot to heel strike.16
The overall goal with orthoses is to improve coordination, balance, posture, and stability during gait, DeCaro said.
For instance, for the typically flexible DS foot, DeCaro said he has found that a functional UCBL (University of California Biomechanics Laboratory) type of orthosis combined with supportive footwear can be effective. He believes all orthoses for children with DS should have a deep heel cup, a medial heel skive, and high medial and lateral sidewall flanges.9
Asked if addressing alignment problems from the feet up in these young patients could potentially prevent hip impairments as they grow older, he replied: “Unequivocally yes! A good foundation is imperative for a lifelong improvement of overall gross motor strength and biomechanics.”
Shalmali Pal is a freelance writer based in Tucson, AZ.
1. Leshin L. Musculoskeletal Disorders in Down Syndrome website. http://www.ds-health.com/ortho.htm. Accessed May 4, 2015.
2. Hip dysplasia. Stanford University School of Medicine website. http://newborns.stanford.edu/HipDysplasia.html#management. Accessed May 4, 2015.
3. Jackson JC, Runge MM, Nye NS. Common questions about developmental dysplasia of the hip. Am Fam Physician 2014;90(12):843-850.
4. Charleton P, Dennis J, Ellis J, et al. Cervical spine disorders: craniovertebral instability. Down Syndrome Medical Interest Group (DSMIG UK). Published March 2012. http://www.dsmig.org.uk/library/articles/CSI%20revision%20final%202012.pdf
5. Caird MS, Wills BPD, Dormans JP. Down syndrome in children: the role of the orthopaedic surgeon. J Am Acad Orthop Surg 2006;14(11):610-619.
6. De la Rocha A, Sucato DJ, Tulchin K, et al. Treatment of adolescents with a periacetabular osteotomy after previous pelvic surgery. Clin Orthop Relat Res 2012;470(9):2583-2590.
7. Katz DA, Kim YJ, Millis MB. Periacetabular osteotomy in patients with Down’s syndrome. J Bone Joint Surg Br 2005;87(4):544-547.
8. Atalar H, Sayli U, Yavuz OY, et al. Indicators of successful use of the Pavlik harness in infants with developmental dysplasia of the hip. Int Orthop 2007;31(2):145-150.
9. Walton MJ, Isaacson Z, McMillan D, et al. The success of management with the Pavlik harness for developmental dysplasia of the hip using a United Kingdom screening programme and ultrasound-guided supervision. J Bone Joint Surg Br 2010;92(7):1013-1016.
10. Pinheiro PC. Nonoperative treatment of slipped capital femoral epiphysis: a scientific study. J Orthop Surg Res 2011;6:10.
11. A patient’s guide to slipped capital femoral epiphysis. OrthoPediatrics website. http://www.orthopediatrics.com/docs/Guides/slipped_CFE.html. Accessed May 4, 2015.
12. Aprin H, Zink WP, Hall JE. Management of dislocation of the hip in Down syndrome. J Pediatr Orthop 1985;5(4):428-431.
13. Adib N, Davies K, Grahame R, et al. Joint hypermobility syndrome in childhood. A not so benign multisystem disorder? Rheumatology 2005;44(6):744-750.
14. Quanbeck D, Greer K, Wilkins K. Joint hypermobility: normal variation or cause of concern? Gillette Children’s Specialty Healthcare: A Pediatric Perspective 2013;22(1):1-3.
15. Martin K. Effects of supramalleolar orthoses on postural stability in children with Down syndrome Dev Med Child Neuro 2004;46(6):406-411.
16. Selby-Silverstein L, Hillstrom HJ, Palisano RJ. The effect of foot orthoses on standing foot posture and gait of young children with Down syndrome. NeuroRehabilitation 2001;16(3):183-193.



 Studies link hip, shoulder function
Studies link hip, shoulder function Effect might increase future OA risk
Effect might increase future OA risk This guide to orthotic devices for people with Charcot-Marie-Tooth (CMT) disease has been a dream of mine for a long time. I was diagnosed with CMT1A at the tender age of 18 months, but didn’t learn about orthotic devices for CMT until 2007, when I started a support group in Atlanta. Up to that point, I thought ankle foot orthoses (AFOs) were for the aged and infirm—something that, at age 35, I didn’t think I was.
This guide to orthotic devices for people with Charcot-Marie-Tooth (CMT) disease has been a dream of mine for a long time. I was diagnosed with CMT1A at the tender age of 18 months, but didn’t learn about orthotic devices for CMT until 2007, when I started a support group in Atlanta. Up to that point, I thought ankle foot orthoses (AFOs) were for the aged and infirm—something that, at age 35, I didn’t think I was. By Robyn Parets
By Robyn Parets “By my age, I should be hobbled,” Seitzer said.
“By my age, I should be hobbled,” Seitzer said. “They were not so great for those teenage years,” he recalled.
“They were not so great for those teenage years,” he recalled. By Robyn Parets
By Robyn Parets Orthotic devices have played a bigger role in Brennan’s life as his CMT symptoms have become more severe over the years, said Kathy, who also has twin 12-year-old daughters who do not have CMT. Brennan becomes fatigued easily, frequently has pain in his feet and hands, and has trouble with weakness in his extremities. For example, his thumb dislocates often and he has difficulty holding a pencil. In school he uses technology, including an iPad with a keyboard, to help him write and keep up in class, said Kathy, who is a third and fourth grade teacher. Perhaps the hardest thing is watching her son come home from school wiped out or just lie on the floor after playing sports.
Orthotic devices have played a bigger role in Brennan’s life as his CMT symptoms have become more severe over the years, said Kathy, who also has twin 12-year-old daughters who do not have CMT. Brennan becomes fatigued easily, frequently has pain in his feet and hands, and has trouble with weakness in his extremities. For example, his thumb dislocates often and he has difficulty holding a pencil. In school he uses technology, including an iPad with a keyboard, to help him write and keep up in class, said Kathy, who is a third and fourth grade teacher. Perhaps the hardest thing is watching her son come home from school wiped out or just lie on the floor after playing sports. “It was pretty cool. I got to do a photo shoot with a [Chicago] Bears player,” Brennan said.
“It was pretty cool. I got to do a photo shoot with a [Chicago] Bears player,” Brennan said. By Jordana Bieze Foster
By Jordana Bieze Foster “If I had to say anything to people with CMT about AFOs, I would say, ‘Don’t wait,’” Covington said. “We think it’s going to be this devastating experience, but in fact it’s just the opposite. There is nothing about my life that my AFOs haven’t impacted in a positive way. I think they’re just the best.”
“If I had to say anything to people with CMT about AFOs, I would say, ‘Don’t wait,’” Covington said. “We think it’s going to be this devastating experience, but in fact it’s just the opposite. There is nothing about my life that my AFOs haven’t impacted in a positive way. I think they’re just the best.” Over time, Covington has become more comfortable disclosing her condition to others—something that was particularly challenging when she reentered the dating world several years ago as a divorcee. Steiner has convinced her that in hot weather it makes sense to wear shorts, but typically she still prefers long pants over skirts or capris and lace-up shoes over sandals for better AFO camouflage.
Over time, Covington has become more comfortable disclosing her condition to others—something that was particularly challenging when she reentered the dating world several years ago as a divorcee. Steiner has convinced her that in hot weather it makes sense to wear shorts, but typically she still prefers long pants over skirts or capris and lace-up shoes over sandals for better AFO camouflage. AFO Mechanics
AFO Mechanics



 AFO Mechanics
AFO Mechanics


 AFO Mechanics
AFO Mechanics










 By Robyn Parets
By Robyn Parets Soon after Robinson turned 50, he began noticing that he was losing his balance often. His hands and legs were much weaker than usual. When he played racquetball, he couldn’t control his swing, and he noticed that his gait was changing. Then he started to trip frequently, and fall down.
Soon after Robinson turned 50, he began noticing that he was losing his balance often. His hands and legs were much weaker than usual. When he played racquetball, he couldn’t control his swing, and he noticed that his gait was changing. Then he started to trip frequently, and fall down. “My confidence level has increased significantly. I have more stability and energy. I would not be able to walk from one side of the house to the other without them. Until they find a cure for CMT, these are a necessity [for me],” Robinson said.
“My confidence level has increased significantly. I have more stability and energy. I would not be able to walk from one side of the house to the other without them. Until they find a cure for CMT, these are a necessity [for me],” Robinson said.



 By Erin Boutwell
By Erin Boutwell



 Long-term pain warrants early ID
Long-term pain warrants early ID