When a child is required to wear ankle foot orthoses (AFOs), his or her clothes have to be more than just cute. Trying to match the logistical requirements of AFOs with fashion concerns and psychosocial development can be a challenge for patients and parents alike.
By Shalmali Pal
In the anthology of cute kid stories, there’s at least one chapter about children and their clothes. There’s the one about the toddler who insists on choosing her outfit, proudly exiting the house in a riot of colors and patterns. Or the kindergartener who refuses to attend school unless he wears his superhero costume. Or the tween who must have the same pair of jeans as her friends, no substitutions allowed.
But when the child is required to wear ankle foot orthoses (AFOs), cute can quickly morph into challenging for patients and parents alike as they try to match the logistical requirements of the AFOs with fashion concerns and psychosocial development. LER checked in with some experts for advice on how to make that match happen and what clinicians can do to help.
Infants, crawlers, and toddlers
For small children (aged 5 years and younger), clothes need to be easy-on, easy-off, whether it’s to facilitate a diaper change or make it more efficient to help the child don and doff the AFOs.
Kathy Martin, PT, DHS, said she’s yet to encounter problems with AFOs related to the type of clothing that is typical for infants, such as baby sacks and onesies.
“It’s not been my experience that parents have to choose different types of clothes based on the braces except that, as with all babies, you want to be able to get them off and on easily,” said Martin, professor and Doctor of Physical Therapy program director at the Krannert School of Physical Therapy at University of Indianapolis. “At that age, kids don’t usually have the manual dexterity or strength to get their braces off, so I don’t think you need special clothing to try to stop them from doing that.”
Lara Hartung, CO, of O&P Labs in St. Louis, MO, agreed.
“I tell the parents of these kiddos that anything that snaps open and closed along the bottom is usually the way to go,” Hartung said, adding that this holds true even if the child requires a brace with an abduction bar to treat clubfoot.
Yaron “Ron” Raducanu, DPM, president of the American College of Foot and Ankle Pediatrics, added the reminder that climate will impact clothing choices. An infant living in a warmer region may be able to get away with short onesies that leave the AFOs uncovered. Climates that call for more coverage may require some experimentation to determine what accommodates the AFOs best.
Regardless of the clothing, “one key with AFOs, especially if they are custom made, is that they should not cause any irritation to the wearer,” said Raducanu, who is in private practice in Philadelphia. “It’s up to the practitioner to make the brace as comfortable as possible. I think it’s more important to get that right than to be too concerned with anything that goes over the brace.”
But what happens when children become mobile? How should parents dress a crawler or toddler who requires AFOs?
In young children, experts say, often the AFO itself is more restrictive than the child’s clothing. But Raducanu reiterated that streamlining the AFOs as much as possible curtails problems with children’s clothing.
“The Velcro can sometimes be troublesome and catch on the AFOs, so that’s something that I check for and try to minimize,” he said. “Also, you have to look at the placement of the buckles and latches, so that they don’t interfere with clothing and cause discomfort.”
As for clothing materials, there are no hard and fast rules. The experts agreed that socks made with moisture-wicking materials are best for regulating sweat. Otherwise, it’s mostly a matter of trial and error, and communicating with the child to see if the items are suitable for the AFOs, comfortable, and appealing.
Of course, if the child is preverbal, traditional communication may be difficult, but family therapist Jillian Pizzi, MA, has ways to manage that. First, she suggested, healthcare practitioners can use dolls or stuffed animals to show the child where the AFOs will be placed and how their clothing will accommodate the braces. Then, once the child has donned the AFOs, the outfit, or both, use the same dolls to ask the child to point out areas where the braces or the clothes are uncomfortable.
Pretending to put the AFOs on the doll first allows the child to “buy in” to the braces, explained Pizzi, who is with South Bay Mental Health in Lowell, MA.
“They will feel more comfortable seeing it done [on the doll] first, and this may enable them to relax a bit,” she said.
Pizzi has a unique perspective on pediatric AFOs–she was diagnosed with distal arthrogryposis and underwent multiple surgeries, starting when she was 10 months old and ending at age 4. She wore AFOs off and on until she was 7 years old. She now works with disabled children at her counseling practice.
Even when children are very young, Pizzi advised building trust by taking the time to explain the devices, and then giving them some say in the clothes they need to adapt to those devices.
“Taking the time to explain, show, demonstrate, and check in with kids helps to strengthen their trust of who is in their environment and what is going on,” Pizzi said.
Growing up with AFOs
As children develop personalities and personal tastes, the issue of making clothing work with AFOs is no longer just about comfort; the focus can shift to what’s socially acceptable to children and their peers.
“I think it was around age six that I started to become aware of clothes and how things matched or how they looked,” Pizzi recalled. “I remember that I had a terrible time with jeans. I wore a lot of stretchy pants or sweatpants.”
Parents and practitioners need to be aware of the balance between doing what is best for the child’s health and allowing the child to have some say in his or her life, Pizzi said.
“Telling a child, ‘I’m going to give you your own voice’ can be very helpful. Kids respond better if they feel they have some sense of control,” she said.
The first place to start that process is with the AFOs themselves. The ability to dress up AFOs with colors, decals, or stickers has been a tremendous boon.
First, it’s an opportunity for the child to be involved in the decision-making process and gain a sense of control by choosing a design or color. It also “makes the brace less medical,” Hartung pointed out. “It allows them to make it more about something fun for a toddler, or something fashionable for an older child.”
Martin said that being able to bring that sense of fun or fashion can even tip the balance in favor of the AFOs in terms of patient compliance.
“I’ve had parents tell me that their child goes to school with the AFOs featuring a cartoon character and other kids say, ‘I want those!’ It almost becomes a personal fashion statement. And if it’s more appealing to the kids, then they are more likely to wear the braces,” Martin said.
For specific clothing choices, trial and error is what the experts advised, and easy-on, easy-off shouldn’t be completely discounted. Annette is the mother of an 8-year-old girl with Charcot-Marie-Tooth disease. Her daughter has worn AFOs for two years, and she’s finding the balance between being independent and learning to work within some of the limits presented by the AFOs.
“She generally wears sweats [or] elastic waistband pants to make it easier for her to use the restroom,” explained Annette, who lives in California. “She does want to assert her independence as she’s growing up; she gets herself dressed. She is learning to adapt and do things differently than everyone else.”
The experts emphasized two points: making the AFOs part of the child’s routine and letting them make decisions—within limits.
“As soon as you can, have them learn that the AFO is part of their daily lives,” is a recommendation that Hartung makes to parents. “If they are involved from the very beginning, it’s not something that is so torturous. It becomes part of their everyday activities.”
An example would be for the parent or caregiver to give a daily review of the process of putting on and taking off the AFOs, even if the child may be too young to fully comprehend what’s happening. And older children can be allowed to put on their AFOs and shoes and socks themselves, rather than making it something mom or dad does to them.
Pizzi suggested starting this process in children as young as 4 or 5 years, and framing the importance of the AFOs within a story.
“In the story, the adult could describe the activities that they are going to be able to do today because the child is wearing the brace,” she said. “Or maybe there’s a special occasion coming up like a birthday or a family event. The parent could talk about how the child will be able to participate in that more easily with their braces on.”
One of the major rules of parenting also applies to kids and their AFOs—children like making decisions, but they also need boundaries, and that includes their clothing options.
“I think it’s important to structure the choices in a specific way,” Martin said. “A parent can say, ‘Do you want to wear the blue socks or the red socks with the braces?’ You didn’t give them a choice regarding the braces at all; it’s understood that the braces will be worn. It’s up to [the adults] to structure the choices so we get the outcomes we want.”
Raducanu suggested that parents avoid the trauma of trips to the mall with younger kids to try on clothes and shoes. Instead, parents should go out and do the shopping themselves, choosing items that they believe will work with the AFOs, and then let the child try on and choose from that selection at home.
Having to return the unwanted items will require an additional trip to the store, but he pointed out that it’s a small price to pay to avoid “a huge battle that’s only going to leave everyone upset and feeling resentful. That can impact the child’s attitude towards the braces.”
OMG: Teens and AFOs
There’s another chapter in that anthology about the rebellious teen. It’s a time when the desire to fit in is paramount, and having to wear AFOs may not fit the bill at all.
“One of the biggest problems with teenagers is compliance,” Hartung said. “They don’t want to wear something that makes them different.”
Once again, the experts agreed that helping teens fit their fashion needs around their AFOs starts with the devices themselves. The use of light, thin materials, for example, can help AFOs fit under trendy skinny jeans or leggings, Hartung said.
“Our goal is to make sure the brace functions properly and that the patient will wear it,” Hartung said.
If a teenage girl is keen on wearing below-the-knee skirts, but the extra material gets stuck on the Velcro closures, Hartung said she would make it a priority to adjust the closure rather than ruling out the clothing item. Another option for some AFO-wearing teens is to switch from a taller brace to one with a lower profile.
Pizzi pointed out that a militant attitude about AFO compliance can be especially hurtful to an adolescent who is already struggling with the usual teen issues beyond the AFOs. In an essay she wrote as an undergraduate at Rivier University in Nashua, NH, Pizzi recounted a day of shopping for clothes with her mother as “somewhat torturous. If the pants are good, the shoes are not, and if the shoes are good, the pants are not. It is a vicious cycle. I cannot win. So, after…the tenth pair of pants that I had tried that day…I had had enough and stormed out of the store.”
So what’s the best way to manage that kind of frustration, anger, and resentment? Pizzi advised that the teen years would be a good time to introduce psychosocial therapy, which can benefit both the patient and the parents.
Parental protectiveness can be heightened when a child requires AFOs. But teenagers are more likely to misinterpret that caring and become less compliant.
“Who wants their parents nagging them constantly, and what parent really wants to be the nonstop nag? I think it’s important to start empowering teens to more fully understand what they could or should do to help themselves live comfortably with their disability,” Pizzi said. “The idea is that the teen can be a bit more proactive or responsible for his own body and the parent can still [offer] support…and step back or out of the protective role.”
Professional counseling is one option, as are support groups and workshops. Pizzi said she found it very cathartic to pen her college essay.
As for those potentially perilous shopping trips, Pizzi summed up her advice in one word: patience.
“When my mom and I would go to the mall, it could take us five hours to find the right shoes or clothes. We just had to accept that it was going to be a slow, steady process. Eventually, we’d find clothes that were cute and functional, but we both had to be willing to put in the time,” she said.
Ultimately, practitioners and parents alike may have to accept that a teen’s AFOs may spend more time in a closet or school locker than they will on the patients.
“At some point, they may stop wearing the AFOs, or wear them out of the house and then take them off the minute they get to school. And you may just have to let that go. The patient needs to make that decision to wear their AFOs,” Raducanu said.
Adaptive apparel
Parents searching online for clothing options for their AFO-wearing children are likely to come across adaptive apparel. These are clothes and shoes that have been specially designed to work with AFOs. Examples include “hatchback shoes,” that allow the back of the shoe to open up so the foot can slide in; longer, seamless socks that are long enough to cover AFOs of varying heights; and pants that snap closed on the sides so that the front “breaks away” rather than having to be pulled down.
Most of these items are not cheap. Socks can cost as much as $10 a pair, while shoe prices generally run between $80 and $100. Our experts were divided on whether adaptive apparel is worth that kind of money.
Hartung expressed reservations, especially given that kids grow out of shoes and clothes so quickly. She also pointed out that AFOs—and the children who wear them—can take their toll on shoes.
“An older child who is on the go may not take the time to put the shoes on and take them off properly. He might try to jam his foot into the shoe, brace and all, and then collapse the back of the shoe,” she said. “If a parent has spent a lot on a specialty shoe, that’s a problem. I’d rather get them into a regular shoe.”
On the other hand, Annette has opted for adaptive shoes for her daughter and, on the whole, considers them a good fit.
“They are expensive—it cost me about eighty dollars-plus to order her a pair of shoes…and it’ll take two to three weeks before we’ll get them. They can be a good investment since they easily fit her braces,” she said. However, Annette warned that shoes styles are limited. “They only have one pink color for girls and a Mary Jane-type shoe.”
Pizzi remembers her mother investing a few hundred dollars in a couple pairs of adaptive shoes.
“They were very expensive, and she knew I’d outgrow them pretty fast,” Pizzi said. “But they were beautiful shoes, and I did wear them without any complaint.”
Shalmali Pal is a freelance writer based in Tucson, AZ.






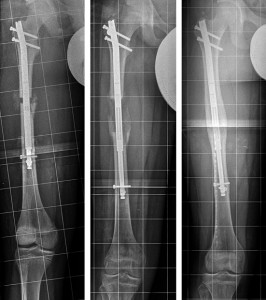
 Position statement cites warning signs
Position statement cites warning signs Second study assesses ‘creep’ risk
Second study assesses ‘creep’ risk
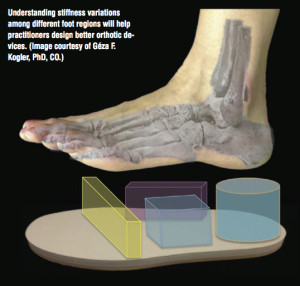


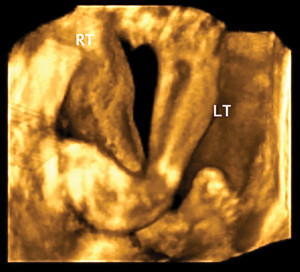
 Some evidence suggests that neuromuscular training before puberty can help further reduce anterior cruciate ligament (ACL) injury rates. But young children respond differently to instruction than their older counterparts, which means early intervention requires some creativity.
Some evidence suggests that neuromuscular training before puberty can help further reduce anterior cruciate ligament (ACL) injury rates. But young children respond differently to instruction than their older counterparts, which means early intervention requires some creativity. “Too many young athletes are specializing in one sport earlier and earlier, in addition to losing time in free play,” said Julie Eibensteiner, DPT, owner of Laurus Athletic Rehab & Performance in Minneapolis, MN. “As a result, kids are lacking the development of physical competence and ability to interact well with their physical environment and self regulate their physical activity.”
“Too many young athletes are specializing in one sport earlier and earlier, in addition to losing time in free play,” said Julie Eibensteiner, DPT, owner of Laurus Athletic Rehab & Performance in Minneapolis, MN. “As a result, kids are lacking the development of physical competence and ability to interact well with their physical environment and self regulate their physical activity.”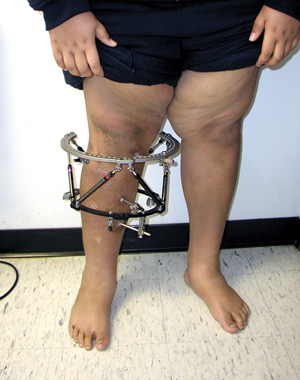

![Robotic training device setup. (Reprinted with permission from Sukal-Moulton T, Clancy, T, Zhang LQ, Gaebler- Spira D. Clinical application of a robotic ankle training program for cerebral palsy compared to the research lab- oratory application: Does it translate to practice? Arch Phys Med Rehabil 2014 May 1. [Epub ahead of print])](http://lermagazine.com/wp-content/uploads/2014/08/8PEDS-CP-figure2-intellistretchMD-copy.jpg)


 The evidence
The evidence Changes
Changes If there’s a practitioner who has redefined the meaning of early intervention, it’s Debbie Strobach, MA, PT, a pediatric physical therapist and splinting specialist at Mercy Children’s Hospital in St. Louis, MO.
If there’s a practitioner who has redefined the meaning of early intervention, it’s Debbie Strobach, MA, PT, a pediatric physical therapist and splinting specialist at Mercy Children’s Hospital in St. Louis, MO. Early intervention can help provide a solid foundation
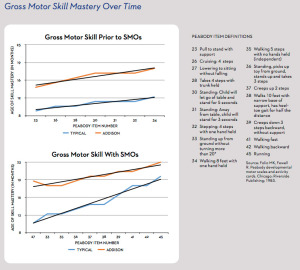
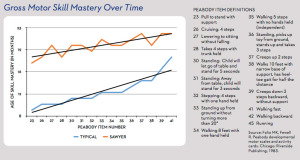
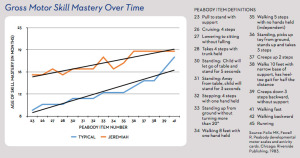
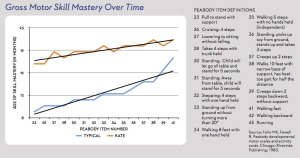
Early intervention can help provide a solid foundation “They pull to stand on time, but then they don’t start cruising within or close to a couple of months of that,” she explained. “Eventually, they may start cruising, but then they get stuck on that; they don’t really let go [of the support]. Parents will often say, ‘They don’t seem to be getting anywhere.’ Then it becomes a bit of a waiting game to see if they progress.”
“They pull to stand on time, but then they don’t start cruising within or close to a couple of months of that,” she explained. “Eventually, they may start cruising, but then they get stuck on that; they don’t really let go [of the support]. Parents will often say, ‘They don’t seem to be getting anywhere.’ Then it becomes a bit of a waiting game to see if they progress.” Building trust is particularly important for working with these patients. While healthcare professionals are no doubt pressed for time, MacFarlane and Smith suggested starting slowly.
Building trust is particularly important for working with these patients. While healthcare professionals are no doubt pressed for time, MacFarlane and Smith suggested starting slowly.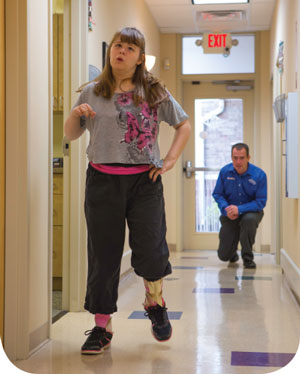 Quantifying the effects of hypotonia starts in the clinic
Quantifying the effects of hypotonia starts in the clinic “The patient will walk perfectly in the lab, but then the parents say, ‘Oh no, they don’t walk like this at home,’” he said. “It’s ironic, because ideally what we want is for them to walk imperfectly in the lab so we can help them walk perfectly outside of the lab.”
“The patient will walk perfectly in the lab, but then the parents say, ‘Oh no, they don’t walk like this at home,’” he said. “It’s ironic, because ideally what we want is for them to walk imperfectly in the lab so we can help them walk perfectly outside of the lab.” The reading
The reading The two conditions were associated with different gait strategies. Patients with PWS showed some functional limitations at every level of the lower limb joints, whereas those with EDS had greater limitations that were nevertheless found mainly at the distal joints.
The two conditions were associated with different gait strategies. Patients with PWS showed some functional limitations at every level of the lower limb joints, whereas those with EDS had greater limitations that were nevertheless found mainly at the distal joints. Even though research into pediatric flexible flatfoot (PFF) is sometimes used as a proxy given the scarcity of data about hypotonia and hypermobility, the clinicians LER spoke with for this article generally downplayed the idea of a correlation. Depending on severity and factors such as patient and clinician preferences, most cases of PFF are treated with watchful waiting or simple orthotic strategies. And PFF is not, in any case, a neurological condition.
Even though research into pediatric flexible flatfoot (PFF) is sometimes used as a proxy given the scarcity of data about hypotonia and hypermobility, the clinicians LER spoke with for this article generally downplayed the idea of a correlation. Depending on severity and factors such as patient and clinician preferences, most cases of PFF are treated with watchful waiting or simple orthotic strategies. And PFF is not, in any case, a neurological condition.
 In the 1970s, neurologists began classifying types of hypotonia, but “benign congenital hypotonia” remained a diagnosis when no cause could be found. Improvements in identifying genetic, neuromuscular, and connective tissue disorders now provide more detailed answers, opening the door to appropriate treatment responses. Still, some families live with the frustration of knowing hypotonia exists without discovering its underlying cause.
In the 1970s, neurologists began classifying types of hypotonia, but “benign congenital hypotonia” remained a diagnosis when no cause could be found. Improvements in identifying genetic, neuromuscular, and connective tissue disorders now provide more detailed answers, opening the door to appropriate treatment responses. Still, some families live with the frustration of knowing hypotonia exists without discovering its underlying cause. Hypotonia is a common feature of genetic disorders associated with developmental delay. Children with Angelman syndrome have gait ataxia with tremulous limbs, but may not always have hypotonia.9 Neonates with Prader-Willi syndrome (PWS), however, have severe hypotonia, evidenced by lethargy and weak or no sucking. As children grow, their gross motor skills are typically delayed; they may sit at 12 months and walk at 24 months, though in some cases walking may be delayed until they are aged 4 or 5 years.
Hypotonia is a common feature of genetic disorders associated with developmental delay. Children with Angelman syndrome have gait ataxia with tremulous limbs, but may not always have hypotonia.9 Neonates with Prader-Willi syndrome (PWS), however, have severe hypotonia, evidenced by lethargy and weak or no sucking. As children grow, their gross motor skills are typically delayed; they may sit at 12 months and walk at 24 months, though in some cases walking may be delayed until they are aged 4 or 5 years. In caring for patients with low muscle tone or ligament laxity, Cusick relies on management strategies that improve functioning joint alignment and raise the level of—and improve the quality of—sensory input in daily life. To support these goals, she developed TheraTogs, a live-in orthotic undergarment and strapping system for children with hypotonia and other issues that is designed to deliver enhanced sensory input and improve postural alignment, and can be used in conjunction with orthotic devices that specifically target the foot and ankle. She also selects play activities that build balancing skills, muscle strength, and muscle tone, while maintaining the feet, trunk, and hips in optimum alignment.
In caring for patients with low muscle tone or ligament laxity, Cusick relies on management strategies that improve functioning joint alignment and raise the level of—and improve the quality of—sensory input in daily life. To support these goals, she developed TheraTogs, a live-in orthotic undergarment and strapping system for children with hypotonia and other issues that is designed to deliver enhanced sensory input and improve postural alignment, and can be used in conjunction with orthotic devices that specifically target the foot and ankle. She also selects play activities that build balancing skills, muscle strength, and muscle tone, while maintaining the feet, trunk, and hips in optimum alignment. “Enriching and transforming lives through compassionate care and innovation” is our company mission statement. As our focus is on the pediatric special needs population, it’s pretty easy to stay attentive to that mission. Still, we know we can only make a difference in the lives of our patients with the dedication of our employees to our mission and the culture we strive to achieve. Our culture is the “compass” that guides us.
“Enriching and transforming lives through compassionate care and innovation” is our company mission statement. As our focus is on the pediatric special needs population, it’s pretty easy to stay attentive to that mission. Still, we know we can only make a difference in the lives of our patients with the dedication of our employees to our mission and the culture we strive to achieve. Our culture is the “compass” that guides us.






